Differences in healthcare resource utilization by race/ethnicity among moderate to late preterm infants with respiratory distress Syndrome, Northern California
In this study, we evaluated racial and ethnic disparities in HCRU among moderate to late preterm infants with RDS. While HCRU during birth hospitalization was largely similar across racial and ethnic groups, disparities emerged in the first year of life. Black and Hispanic infants had significantly higher rates of ED visits within the first year of life when compared with White infants. While hospitalization rates were similar across Black and White infants, Hispanic infants had significantly higher odds of respiratory-related hospitalizations.
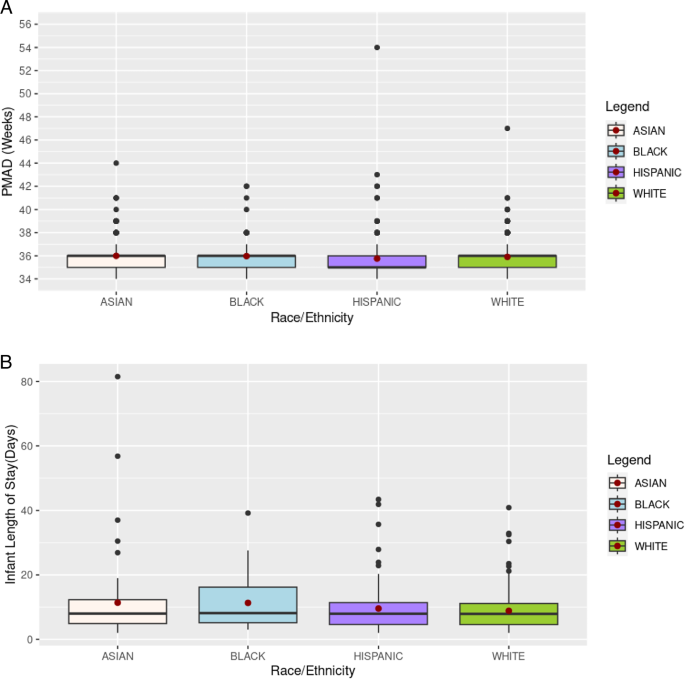
We did not observe racial/ethnic disparities among outcomes during birth hospitalization including LOS and respiratory support, potentially due to our homogenous clinical population including infants with RDS and using a single integrated healthcare system implementing standardized protocols for early respiratory management. A large nationally representative study of over 80,000 late preterm infants (33-36 weeks’ gestation) examined demographic and clinical predictors of hospital LOS. This study found gestational age, sex, birthweight and clinical complications including RDS, sepsis and necrotizing enterocolitis were stronger predictors of longer LOS than race [16]. These findings suggest that clinical factors may play a greater role than sociodemographic factors in short-term outcomes during birth hospitalization. Other studies have reported racial and ethnic disparities in pediatric HCRU, including one study suggesting that Black, Hispanic, and other minorities experience longer LOS for pediatric conditions, even after accounting for clinical and demographic factors [17]. However, this study focused on a broader pediatric population (children <21 years), including common diagnoses like pneumonia and bronchiolitis rather than newborn-specific conditions such as RDS. The study also encompassed a wide range of hospital settings including rural and urban teaching and non-teaching hospitals, which may contribute to variability in care delivery and a lack of standardized treatment protocols, potentially leading to the observed differences. Additionally, in a large national cohort of over 219,000 infants born at 22-29 weeks’ gestation, Boghossian et al. [2019] observed racial and ethnic disparities in hospital outcomes including mortality and morbidity[12]. Although disparities narrowed over time for some outcomes, rates of hypothermia, LOS, and mortality remained elevated, particularly for Black infants. These differences likely reflect variability in care across NICUs, especially in minority-serving hospitals and the greater complexity and duration of care for this less mature patient population. Similarly, racial disparities in short-term outcomes such as LOS and mortality have been observed among infants with bronchopulmonary dysplasia (BPD), even after accounting for severity [18]. However, unlike our study, which focused on a single, acute condition with standardized treatment protocols, BPD is a chronic condition with variation in management. These differences in clinical course and management protocols in BPD likely contributed to greater variability in care and outcomes. Overall, previous studies show conflicting results related to short-term outcomes. In contrast to prior studies involving chronic conditions and varied care settings, our study focused on RDS, an acutely managed condition with standardized treatment, within a single healthcare system, potentially representing more consistent care standards and therefore fewer disparities observed among short-term outcomes.
While racial and ethnic disparities in HCRU were not observed during birth hospitalization, significant differences across ED visits and hospitalizations were observed post-discharge. These findings are consistent with prior research on ED visit recidivism and hospital readmission rates in pediatric populations, likely occurring because of access to care and overall systemic inequities that disproportionately affect Black and Hispanic infants [19,20,21]. LeDuc et al. (2005) reported increased odds of ED return visits among Black and Hispanic infants, primarily due to limited availability of primary care providers [20]. Within a California cohort, Karvonen et al. (2021) found Black and Hispanic MLPT infants to experience higher post-discharge mortality and hospital readmission rates compared to White infants despite having lower mortality while in hospital [21]. These differences were likely attributed to reduced access to both primary and subspecialty care post-discharge, financial limitations, and lower adherence to follow-up appointments [21, 22].
Although both Black and Hispanic infants had greater risk of ED visits post-discharge, only Hispanic infants showed greater risk of hospitalizations. In a similar study, Hispanic infants had the highest adjusted risk of rehospitalization during the first year of life [23]. These disparities may reflect differences in the utilization of preventive or follow-up care and the management of respiratory symptoms after discharge, rather than differences in access alone. For example, Hispanic preterm infants were found to be significantly less likely than White infants to receive treatment for respiratory symptoms after discharge whereas Black infants were more likely to receive these treatments, regardless of severity of symptoms [24]. This potential underutilization of respiratory treatment may contribute to a higher risk of complications requiring hospitalization. Additionally, Hispanic individuals have been found to experience greater challenges in accessing healthcare, including difficulty finding providers and greater transportation barriers, compared to both White and Black individuals [25, 26]. Despite all infants in this study having medical insurance through KPNC, racial and ethnic disparities in outcomes persisted.
Structural racism may play an important role in contributing to these disparities. Black preterm infants living in areas of greater racial and economic disparities tend to have increased risks of acute care visits, rehospitalization, and post-discharge mortality even after adjusting for clinical and sociodemographic factors [27]. Although we account for neighborhood deprivation in our study, the NDI may not fully capture residential segregation and structural factors such as limitations in the built environment and access to healthcare. Similar to our findings, previous studies suggest an unlikely trend among Black infants who are at a reduced risk of having respiratory complications in the NICU but experience higher rates of these complications and reduced lung function after hospital discharge [28]. This shift post-discharge likely results from impacts of experiences beyond the NICU, where minority infants face greater exposure to environmental hazards, reduced access to preventive respiratory care, impacts by insurance coverage, and other adverse conditions that may worsen these chronic respiratory conditions [21, 23, 29].
This study has several strengths, including the use of a large, diverse population from an integrated healthcare system in California, allowing for detailed assessment of racial and ethnic disparities in HCRU. Additionally, the inclusion of both short-term and long-term outcomes provides a comprehensive look at disparities beyond the neonatal period. However, there are limitations to consider. First, our study was conducted within a single healthcare system, which may limit generalizability to other settings. Second, while we adjusted for gestational age, NDI, and infant sex, unmeasured confounders, such as individual socioeconomic position, may contribute to the disparities observed. Third, the study period (January 2019 to December 2023) included both the COVID-19 pandemic and the 2022-2023 “tripledemic” of COVID-19, RSV and influenza, which may have influenced healthcare seeking behavior (e.g., vaccination, telehealth) or differential viral exposure risks by race/ethnicity. To evaluate its impact on the findings, we conducted a sensitivity analyses evaluating the racial/ethnic disparities in outcomes by both pre- and post- periods for both the pandemic and tripledemic. We found that the direction and magnitude of generally remained consistent, suggesting these events did not impact observed patterns in this population. Additionally, three infants died between discharge and one year and did not contribute data for outcomes beyond their time of death. Given the small number of deaths, the impact on overall estimates is likely minimal. Finally, because our analysis includes follow-up of infants after discharge, there is potential for selection bias due to differences in loss to follow-up by race/ethnicity. In supplemental analyses, we observed that Black infants had shorter follow-up time compared to White infants. These differences may potentially bias findings towards the null. Overall, it is important to note that race and ethnicity are social constructs used to capture the differences in exposures likely attributed to structural racism. Because these categories include diverse populations with different risk factors and healthcare experiences, this study may not fully capture individual experiences.
link




