A Different Kind of Care

The compelling case for palliative care in advanced kidney disease
Advanced kidney disease requires some of the most complex care in medicine due to medical management, comorbid conditions, symptom burden, patient and family psychosocial needs, difficult conversations, and advance care planning.
Despite the significant coordination needed, care for this patient population is often more fragmented, with less access to supportive services, than for people with other chronic, life-limiting illnesses. For example, oncology and cardiology have addressed similar challenges by establishing and integrating palliative care models. Many are calling for similar models in nephrology.
The Center to Advance Palliative Care (CPA-C) recently partnered with the National Kidney Foundation to publish “The Case for Palliative Care in Kidney Care.”1 The document argues for the “critical need to integrate palliative care services into the treatment of patients with advanced kidney disease.” It calls on nephrology professionals to seek training in palliative care skills and collaborate with palliative care specialists.
Some practitioners believe that the need is so great that they have taken it upon themselves to become certified in both. Nurse practitioner Christine Corbett, DNP, worked in nephrology for more than 20 years and then decided to pursue additional specialty certification in palliative care.
“Patients with kidney disease often face a significant symptom burden, fear, and anxiety related to the disease, and a sense of failure as the disease progresses,” said Corbett, executive director of the Coalition for Supportive Care of Kidney Patients and an assistant research professor at George Washington University School of Nursing. “I saw a huge care gap in my practice and chose to merge these two specialties to provide additional, much-needed support to my patients and their families.”
Palliative care offers a vital, yet often underutilized, dimension to the management of advanced kidney disease. Despite its proven benefits in improving quality of life and aligning treatment with patient goals, nephrology has historically been slow to integrate it into standard practice. Understanding the barriers, alongside practical strategies for cultivating palliative care expertise, can help clinicians provide care that is both compassionate and clinically sophisticated.
Common Misperceptions About Palliative Care
One of the main reasons patients with advanced kidney disease do not regularly receive palliative care is that the public and many healthcare professionals still fundamentally misunderstand what it is. They often fail to recognize the distinct differences between palliative care and hospice care.
Hospice care is a supportive approach to care for people with terminal illnesses who have a life expectancy of 6 months or less. It focuses on comfort and quality of life instead of a cure.
Palliative care focuses on improving decision-making and quality of life for people living with serious illnesses. It can be applied regardless of prognosis and at any stage of illness. Importantly, it can co-occur with curative treatments.
Allison Silvers, chief healthcare transformation officer at CAP-C, explains: “It’s important that nephrology professionals understand what palliative care is: an added layer of support for patients and families as they manage their illness. This is specialized, team-based care that focuses on providing relief from the symptoms and stresses of the illness, with the goal of improving quality of life.”
Wanting to gauge their understanding of palliative care, CAP-C surveyed the public and physicians in 2011 and again in 2019. Although physician awareness improved over the 8 years between surveys, confusion persisted.2 Public awareness did not improve.
“Many have the false belief that palliative care is only for the end of life. CAP-C does our best to fight against that, because it’s just not true. But it’s very difficult to move that needle,” Silvers said. “With dialysis, renal failure isn’t often thought of as a ‘terminal illness.’ And because of the conflation with end-of-life care, many believe that you can’t get both dialysis and palliative care—which is not true! But this might interfere with many dialysis professionals recommending palliative care.”
Lack of Education and Certification in Palliative Care
Education and certification are also significant barriers to the regular use of palliative care in advanced kidney disease.
“There are many reasons, and they start with a lack of formal—or even informal—education for nephrology providers in primary palliative care skills, shared decision-making, and values-based care within their medical school, residency, fellowship, and nursing programs,” Corbett said. “With lack of awareness and lack of training in primary palliative care skills, there tends to be lack of patient support and referral to palliative care.”
Furthermore, Silvers said, palliative care is a subspecialty, and very few physicians or nurses are double certified in nephrology and palliative care, compared with oncology and cardiology. She added that oncology has better-integrated palliative care because palliative care programs were largely founded, developed, and studied at academic cancer centers.
The “Dialysis Default” and the Nature of Nephrology Practice
Corbett also points to a “dialysis default” in the United States. “We often presume patients want all aggressive treatment options, such as dialysis, but without holding those conversations, we may not understand that patients often prefer improved quality of life over longevity. Significant research supports this. Many clinicians are not prepared to hold those conversations or to support patients when those conversations arise,” she said.
Complicating this issue is the nature of nephrology practice. Patients are often referred to nephrology late in the care continuum, often after being managed for a while by primary care. In such cases, care becomes a more critical intervention rather than a support pathway with a focus on quality of life.
Once patients are under nephrology care, they often find themselves in busy clinics or hospitals that are fast-paced and task-based. Taking time to implement the key components of palliative care can seem time-consuming or daunting, Corbett said.
Systemic Barriers and Inequities
This complex issue becomes even more complicated when considering systemic barriers, such as reimbursement and healthcare inequities.
“Medicare’s End-Stage Renal Disease Quality Incentive Program for dialysis facilities does not consider symptom burden or symptom control in its quality measures, nor anything to do with patient decision-making,” Silvers said. “In fact, one of the key clinical measures, kt/V, encourages facilities to maximize dialysis sessions, even when fewer sessions may improve quality of life and better align with patient goals.”
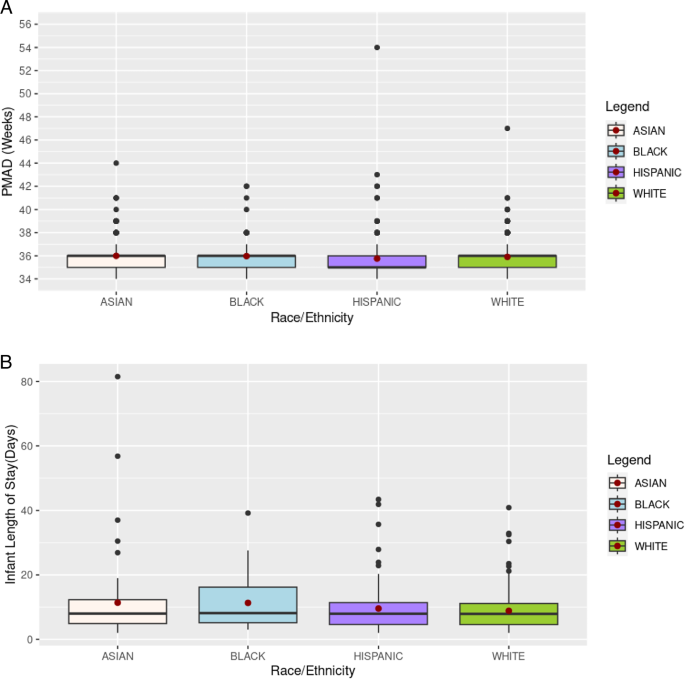
Racial inequities also may play a significant role. Black, Hispanic, Asian, and Native American people are disproportionately affected by kidney disease, and studies have shown that those populations are less likely to have conversations with healthcare professionals about their priorities.3, 4
Reaping the Rewards of Palliative Care in Nephrology
Silvers and Corbett emphasized that the literature shows that the effort required to integrate palliative care into nephrology is worth it. Benefits include the following:1
- Reduced healthcare utilization and costs: Studies have shown that palliative care can reduce emergency department visits, hospital admissions, rehospitalizations, length of stay, the need for intensive care, and healthcare costs.4,5
- Enhanced medical decision-making: Palliative care helps patients and families understand their treatment options and assess what best aligns with their personal goals and values.
- Coordination of care: Palliative care specialists can help coordinate care between nephrologists and other specialists, which is especially important among patients with advanced kidney disease, who often have concomitant conditions.
- More effective symptom management: A palliative approach can enhance attention to and management of kidney symptoms such as pain, fatigue, insomnia, nausea, dyspnea, and pruritus.
- Psychological and emotional support: This level of care can help alleviate anxiety, fear, and depression, often associated with serious illness. Palliative care also supports family members and caregivers with education, communication, decision-making, and stress management.
- Improved quality of life: By improving symptoms and mental health, palliative care can help patients participate more fully in activities of daily living and social events.
- Advance care planning: Palliative care encourages patients and families to prepare for the future and document any end-of-life wishes.
Where to Gain Palliative Care Skills
With some training, the kidney care team can provide basic palliative care, although more complex cases warrant consultation with a specialty palliative care team. For those who want to build their palliative care skills, Silvers and Corbett offered several resources.
“Prognostication tools are imperative to understanding disease trajectory and discussing that with patients and their families so that they are well-informed. Many nephrology providers are unaware of prognostication tools or guidelines, such as the Renal Physicians Association’s guideline, ‘Appropriate Initiation of and Withdrawal From Dialysis.’”
Other resources include:
It can be surprisingly simple to start, Corbett noted. “I ask patients open-ended questions, and often they are willing to provide what is needed in a short amount of time.”
“I think the big lesson is to screen for palliative care needs. Remember to ask about symptom burden—fatigue, pain, etc. And, also, ask about caregiver burden,” Silvers said. “I feel we are finally near a culture shift, with many providers thinking differently about the care they provide.”
link